Right vs Left SI Joint Pain in Pregnancy and Postpartum: Causes and How to Fix It
Pelvic pain during pregnancy and postpartum is incredibly common, but it is often misunderstood and incorrectly treated. One of the biggest missing pieces when addressing SI joint pain is understanding that right sided and left sided pelvic pain are often caused by different movement patterns.
If you have been dealing with SI joint pain during pregnancy, postpartum pelvic pain, or one-sided hip and back pain, this guide will help you understand why it is happening and how to actually fix it.
What Is Pelvic Pain?
Pelvic pain is discomfort in the pelvic region that can show up in a few different areas. You may feel it in the front of the pelvis at the pubic symphysis, or in the back near one or both SI joints.
Many people describe pelvic pain as:
- SI joint pain
- Pubic symphysis pain (SPD)
- Sciatic or piriformis pain
- Tailbone discomfort
- Lower back or deep hip pain
Pelvic pain is often worse during single leg movements like walking, climbing stairs, getting dressed, or rolling in bed. These movements require the pelvis to shift and stabilize, which is where dysfunction tends to show up.
What Causes SI Joint Pain in Pregnancy and Postpartum?
The two main contributors to pelvic pain are form closure and force closure, and understanding both is key if you want to actually resolve SI joint pain instead of just managing symptoms. Most people are only told to rest or wear a brace, but that does not address how the pelvis is moving and stabilizing.
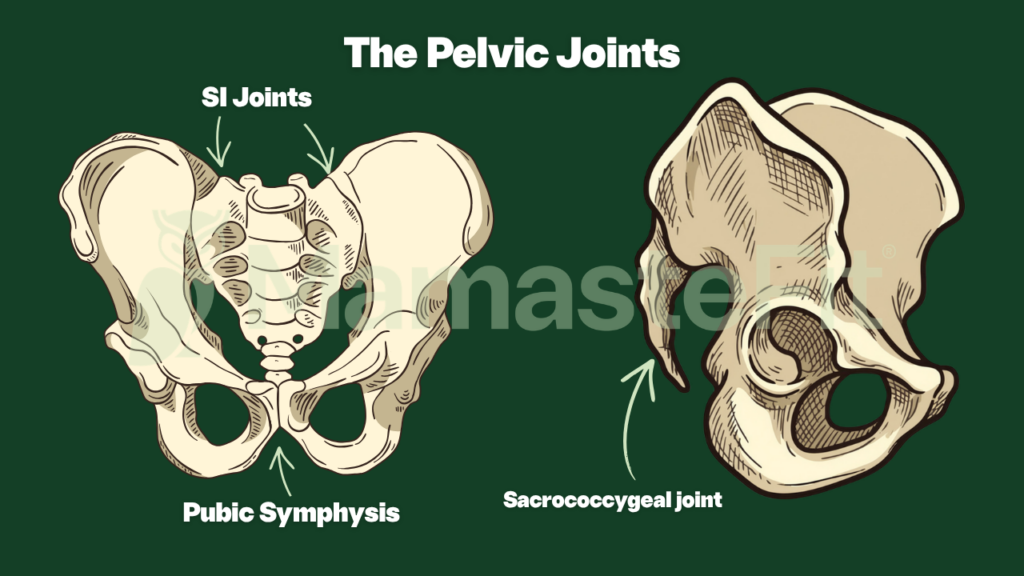
Your pelvis is made up of two pelvic halves and a sacrum, connected by four joints: the pubic symphysis in the front, the two sacroiliac (SI) joints in the back, and the sacrococcygeal joint between the sacrum and tailbone. These joints are designed to move slightly, and while that movement is small, it plays a huge role in how your body transfers load during daily movement.
Form Closure: Pelvic Balance and Mobility for Pelvic Pain
When you walk, shift weight, or move from one leg to the other, your pelvic halves and sacrum are constantly adjusting position. This allows your body to distribute force efficiently, but if that movement is limited or the pelvis gets “stuck” in one position, it can start to create irritation and pain.
This is where form closure comes in. Form closure refers to how well the pelvic joints align and shift during movement, which is essential for creating a stable base when you are standing or moving on one leg.
For example, when you shift your weight into your right leg, the right pelvic half should internally rotate, adduct, and slightly posteriorly tilt to help stabilize your body. When you shift into your left leg, that same pattern should occur on the left side.
If the pelvis cannot move into these positions, or if one side has difficulty shifting, it can impact how well the joints align. Over time, this can contribute to SI joint pain, pelvic girdle pain, pubic symphysis pain, or discomfort in the hips and lower back.
Force Closure: Myofascial Sling Support for Pelvic Pain
The second piece is force closure, which refers to how well the surrounding muscles support and stabilize the pelvis during movement. Even if the joints are able to move, they still need muscular support to control that movement and keep the pelvis stable under load.
Force closure is largely driven by the coordination of the myofascial slings, which are systems of muscles that cross the pelvis and connect the upper and lower body. These slings work together to create tension across the pelvis and help bring the joints together for stability.
If these slings are not working well together, or if there is an imbalance within a sling, it can disrupt how the pelvis stabilizes. This can lead to increased strain on the SI joints and contribute to ongoing pelvic pain.
So when we are trying to resolve pelvic pain, we need to look at both sides of the equation. We need the pelvis to move well and shift between positions, and we need the muscles to support and stabilize those movements.
This is why we focus on three key areas:
- Pelvic mobility, so the joints can move and reposition
- Pelvic balance, so both sides can share load appropriately
- Myofascial sling strength, so the pelvis is supported during movement
This approach goes beyond just managing symptoms and instead addresses the root cause of pelvic pain. It is also why so many of our clients are able to find relief, sometimes even within a single session, once their body starts moving and stabilizing more effectively.
Right vs Left SI Joint Pain: Why It Feels Different
When it comes to resolving SI joint pain, whether your pain is on the right side or the left side will influence how we approach it. The general strategy is similar, and doing work for both sides is usually helpful, but when you understand what each side actually needs, you can be much more deliberate and often find relief faster.
In my own pregnancies, I tend to experience more right sided SI joint pain. When I consistently apply this approach, I can usually calm symptoms down within the same day because I am addressing the underlying pattern instead of just trying random stretches or exercises.
How Your Pelvic Changes Position in Movement
To understand why the right and left sides feel different, we need to go back to how the pelvis is supposed to move. As we walk or shift weight, the pelvis is constantly alternating between sides to transfer load and create stability.
When you shift your weight into one leg, that side becomes your stance leg and should move into internal rotation, adduction, and a slight posterior pelvic tilt. This helps that side of the pelvis stabilize your body while the other leg moves through space.
At the same time, the opposite side, or your swing leg, should move into external rotation, abduction, and a slight anterior pelvic tilt. This alternating pattern allows you to move efficiently and keeps the pelvis balanced between mobility and stability.
This pattern continues with every step you take, and ideally, both sides of the pelvis can move in and out of these positions without restriction.

Your Pelvis Has Normal Asymmetry
Another important piece to understand is that our bodies are not perfectly symmetrical. Our internal organs are not evenly distributed, and our diaphragm is larger on the right side, which tends to make the right side feel more stable.
Because of this, most people naturally shift more weight into their right leg when they stand. This is a normal pattern and not a problem on its own, but if you are dealing with pelvic pain, it often means you are getting “stuck” in this pattern and not able to shift out of it effectively.
So instead of the pelvis alternating smoothly between sides, one side may be doing too much work while the other is not doing enough. This is where we start to see differences between right sided and left sided SI joint pain.

Right Side SI Joint Pain: Stuck in a Loaded Position
Right sided SI joint pain is often related to spending too much time in the right stance position. Because this side already tends to feel more stable, it is easy to default into it and rely on it more during standing and movement.
Over time, this can lead to the right pelvic half staying in a more internally rotated, adducted, and posteriorly tilted position. Instead of being able to move in and out of this position, it becomes the place your body lives.
When this happens, the tissues on the front and inside of the pelvis, especially the right anterior pelvic floor, can become overactive. These muscles are constantly working to stabilize, which can lead to tension, fatigue, and eventually irritation.
This is why right sided SI joint pain is often associated with:
- Hip impingement or pinching in the front of the hip
- Tightness in the groin or hip flexors
- Bladder urgency or pressure
- A feeling of being “stuck” in the right hip
The issue here is not that the right side is weak, but that it has lost its ability to move out of its default position. It needs variability, not more stability.
To address right sided SI joint pain, the goal is to:
- Reduce excessive tone in the right anterior pelvic floor
- Create space for the pelvis to move out of internal rotation
- Restore external rotation, abduction, and anterior tilt on that side
This helps the right side come out of its constant stance position so the pelvis can start to alternate more normally again.
Follow along with this workout to help restore movement and relieve right sided SI joint pain:
If this is helpful and you want more guidance, come join us on YouTube. We share weekly workouts for pregnancy, postpartum, and pelvic floor health, and you can start with our pelvic pain relief playlist here to follow along right away.
Left Side SI Joint Pain: Difficulty Stabilizing Under Load
Left sided SI joint pain tends to be a different problem. Instead of being overused, the left side often struggles to fully accept load and stabilize when you shift weight onto it.
If your body prefers to stay on the right side, it may avoid fully shifting into the left leg. When this happens, the left pelvic half does not consistently move into internal rotation, adduction, and posterior tilt when it needs to.
This can make the left side feel unstable, especially during single leg activities like walking or standing. The body may try to compensate by tightening surrounding muscles, which can lead to discomfort in the glute or deep hip.
This is why left sided SI joint pain is often associated with:
- Glute pain or deep hip discomfort
- Piriformis tightness
- Sciatic type symptoms
- Difficulty balancing or trusting the left leg
In this case, the issue is not that the left side is too tight or overused, but that it is not effectively creating stability when it needs to.
To address left sided SI joint pain, the goal is to:
- Improve your ability to shift weight into the left leg
- Build strength in positions that support internal rotation and adduction
- Help the pelvis find a stable position on that side
This allows the left side to actually do its job during movement instead of relying on compensation from other areas.
Follow along with this workout to improve left side stability and relieve SI joint pain:
Whether you are currently dealing with pelvic pain or want to stay ahead of it, our Pelvic Stability Program walks you through exactly how to build mobility, balance, and strength on both sides. With on-demand workouts for pregnancy and postpartum, I coach you through every rep with clear guidance and progressions from beginner to advanced.
How to Fix Pelvic Pain: Exercises for Pelvic Balance and Stability
Now that we understand how pelvic pain is influenced by both form closure (mobility and alignment) and force closure (muscular support), we can break down exactly how to train both.
To truly resolve pelvic pain, we need a combination of:
- Pelvic balance and mobility work to allow the pelvis to shift between positions
- Targeted strengthening to support those positions
- Myofascial sling training to stabilize the pelvis during movement
When these three pieces come together, your pelvis can move well, stabilize effectively, and tolerate daily activities without irritation.
Step 1: Pelvic Balance and Mobility Exercises
Pelvic balance work focuses on restoring the ability for each side of the pelvis to move into the positions it needs for stability. This includes both releasing overactive areas and strengthening underactive ones.
Most people will present with a pattern where the right anterior pelvic floor and left posterior pelvic floor are more overactive. This creates imbalance in how the pelvis shifts and stabilizes.

Right Anterior Pelvic Floor Release
The right anterior pelvic floor is often overactive due to spending too much time in a right stance position. This area includes the inner thigh and groin and can contribute to tension, hip pinching, and bladder pressure.
To address this, we want to reduce tone and create space so the pelvis can move out of that position.
Exercise: Lateral Hip Shifts
Focus on gently shifting your pelvis to the left, thinking about bringing the right hip to the left knee, while allowing the right inner thigh and groin to lengthen and stretch. This helps reduce tension and improve your ability to move out of the right stance pattern.
Left Posterior Pelvic Floor Release
The left posterior pelvic floor, including the deep glute and posterior hip, is often overactive as the body compensates for instability on that side.
This can contribute to glute tightness, piriformis discomfort, and sciatic type symptoms.
Exercise: Hip Shifts
Use controlled pelvic shifting to allow the left posterior hip to relax and reduce excessive tension. This helps the pelvis reposition more effectively when loading the left leg.
Right Posterior Pelvic Floor Strengthening
Once we create space on the right side, we want to build strength in the posterior hip to help the pelvis move into external rotation, abduction, and anterior tilt.
This supports better movement variability and reduces reliance on the anterior structures.
Exercises that focus on external rotation and abduction help to strengthen the posterior pelvic area:
- Hip shifts into external rotation and abduction
- B-stance squats with a right side emphasis
These movements help strengthen the glutes and posterior hip so the right side can move out of its default position and support dynamic movement.
Left Anterior Pelvic Floor Strengthening
On the left side, the focus is building strength in positions that support internal rotation, adduction, and posterior tilt so that side can better accept load.
This helps improve stability during single leg activities.
Exercises:
- Staggered stance RDL with banded adduction
- Adductor side plank
These exercises target the hamstrings and adductors, which play a key role in stabilizing the pelvis when shifting into the left leg.
Step 2: Myofascial Sling Training for Pelvic Stability
Once you improve pelvic balance, the next step is building force closure, which is how your muscles stabilize the pelvis during movement.
This is where myofascial slings come in.
Myofascial slings are groups of muscles that connect the upper and lower body and cross over the pelvis. These slings help transfer force and create stability, especially during dynamic movement like walking, running, and lifting.
When these slings are coordinated, they help “hold” the pelvis together while still allowing movement. If they are not working well together, the pelvis may feel unstable or overloaded.

Anterior Oblique Sling
The anterior oblique sling connects your obliques to the opposite inner thigh. It plays a major role in cross-body stability and helps control rotation through the pelvis.
Exercise: Split Squat March
This movement trains the connection between the core and inner thigh while also challenging single leg stability. Focus on maintaining control as you shift weight and drive the knee upward.
If this variation feels too challenging, you can regress to stepping to a box instead of hovering the leg and omitting the split squat. Our general approach to managing pain with pelvic pain is to decrease overall movement, even the stance, and add more support.
Posterior Oblique Sling
The posterior oblique sling connects your lat to the opposite glute and stabilizes across the SI joint.
Exercise: Reverse Lunge Row
This combines hip extension with an upper body pulling motion, training the sling to co-contract and stabilize the pelvis during movement.
Deep Longitudinal Sling
This sling runs along the back of the body and helps transfer force through the posterior chain.
Exercise: Suitcase Deadlift
Holding weight on one side challenges your body to stabilize and transfer load through one side while maintaining alignment.
Lateral Sling
The lateral sling supports single leg stability and helps control pelvic position during movement. These movements train your ability to stabilize on one leg and maintain pelvic control during loading.
Exercises:
- Step-ups
- Lateral band walks
How to Use These Exercises Together
To fully resolve pelvic pain, we do not just pick random exercises. We use a progression that builds from mobility into strength and then into coordinated movement.
A simple way to approach this is:
- Start with pelvic balance work to reduce tension and restore movement
- Add targeted strengthening to support each side of the pelvis
- Progress into myofascial sling exercises to integrate full-body stability
This progression allows your pelvis to first move better, then stabilize, and finally handle dynamic movement without pain. And this is how we approach it in our pelvic stability program.
How to Modify Exercises for Pelvic Pain
If you are currently dealing with pelvic pain, the goal is not to avoid movement, but to adjust movement so your body can tolerate it while still building strength and stability. This is one of the biggest missing pieces, because many people either push through pain or stop exercising altogether, and neither approach actually solves the problem.
Instead, we want to meet your body where it is and gradually build your tolerance back up.
1. Decrease the Amount of Movement and Complexity
The first way to modify exercises is to reduce how much movement and coordination is required.
For example, a reverse lunge requires single leg stability, forward and backward movement, and coordination between both sides of the body. If that feels painful or unstable, you can scale it back.
Start with a split squat, where your feet stay in place but you are still in an uneven stance. This gives you two points of support while still challenging each side differently.
If that still feels like too much, you can bring your feet together into a squat, where both legs are working evenly. This removes the asymmetrical demand and allows you to build strength in a more supported position.
This progression allows you to:
- Maintain the movement pattern
- Reduce instability
- Gradually build back into single leg work

2. Add More Support
Another way to modify is by increasing how much support your body has.
If you are finding lower body exercises cause pain, you can add more support to the exercise:
- Add external support like holding onto a wall or surface
- Squat to a box for more support at the bottom
- Hold onto rings or a sturdy structure as you lunge or squat

3) Add More Activation
You can also add in more activation with bands or a foam roller to help with pelvic stability. The inner thighs play a large role in pelvic stability, so adding some activation can help them work a little more.
You can try adding a band around the inner thigh in your squats or lunges, or pressing the inner knee into a foam roller.

Putting It Into Practice
If you are dealing with pelvic pain, the key is consistency and progression. Doing a few random stretches or exercises may help temporarily, but lasting relief comes from addressing both mobility and stability together.
If you want a structured plan that walks you through this step by step, our Pelvic Stability Program includes all of these exercises with guided coaching, follow-along videos, and clear progressions from beginner to advanced.
Inside the program, I cue you through every rep so you know exactly what to feel and how to progress, whether you are pregnant, postpartum, or returning to fitness.


