Welcome to Moments with MamasteFit! In this new podcast series, we will be discussing one case study every week from our professional experience as a labor nurse and birth doula. In this episode, the focus is on how a baby’s position, particularly the occiput posterior (OP) or occiput anterior (OA), can impact the second stage of labor, known as pushing. The episode breaks down the rotational positions of babies, the challenges posed by an OP position, and the potential need for instrument-assisted delivery such as forceps or vacuum. The show shares insights from a doula and labor nurse, including signs of an OP baby, intervention strategies like inversions and open hip positions, and the importance of understanding the pros and cons of different delivery options for future pregnancies. Practical advice for expecting mothers and their partners is provided to help navigate labor challenges and make informed decisions about childbirth.
The Impact of Baby Position on Labor
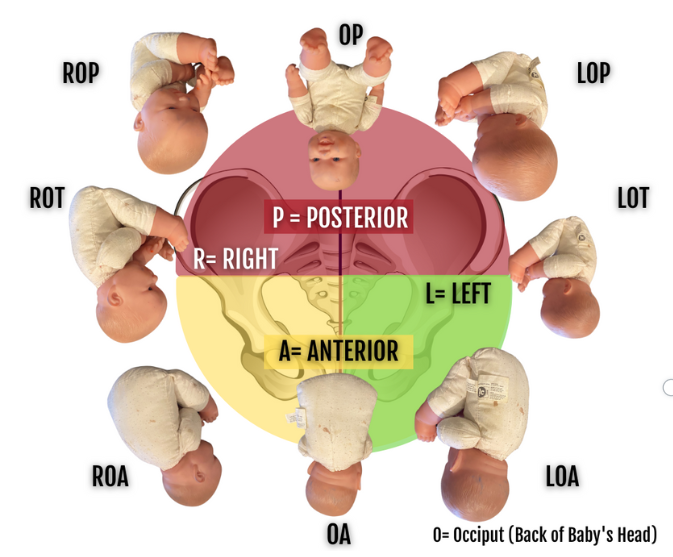
Occiput Anterior vs. Occiput Posterior
In a typical labor scenario, most babies are in the occiput anterior (OA) position, where the back of the baby’s head is aligned with the front of the mother’s pelvis. This alignment facilitates a smoother extension of the head under the pubic arch during the pushing stage. However, when a baby is in the occiput posterior (OP) position—where the back of the head faces the back of the pelvis—it can create challenges.
Key Differences:
OA Position: Baby’s head extends directly under the pubic arch, making the final rotation straightforward.
OP Position: The baby must first tuck its chin and execute additional maneuvers, making the extension more challenging and often prolonging the pushing stage.
Recognizing the Signs
While an OP position can be associated with a longer pushing phase and increased intervention, it’s not always a dire scenario. Some of the signs that indicate a potential OP presentation include:
Early Urge to Push: Mothers may feel an early and persistent urge to push even before full dilation. This is due to increased pressure on the posterior pelvic floor.
Bumpy Contraction Patterns: Contractions that feel like they have multiple peaks or a “tighten, release, tighten, release” rhythm may suggest that the baby is working hard to rotate into an optimal position.
Physical Discomfort: An increased arching of the back during pushing might be an intuitive response to help create space in the pelvic outlet.
Interventions and Strategies
Instrument-Assisted Delivery
When the baby remains in an OP position and labor progress slows significantly, providers might suggest instrument-assisted delivery. I attended a birth where after a prolonged pushing stage, the midwife recommended forceps delivery over a vacuum. The reasoning is that while vacuums are effective when the baby is in an OA position, forceps can be more efficient at guiding a baby in a less optimal (OP) position out of the birth canal. However, the decision between using forceps, a vacuum, or even opting for a Cesarean section depends on multiple factors, including:
The mother’s current labor progress
Future birth options (as a C-section might limit options like home birth with licensed midwives)
Personal preferences and comfort with interventions
Techniques to Encourage Optimal Positioning
Even before reaching the point of instrument-assisted delivery, there are several strategies that can support the baby’s rotation into a more favorable position:

Inversions:
Forward-Leaning Inversion: A steep forward-leaning position (around a 45-degree angle) can help by releasing uterine ligaments and providing additional room for rotation.
Puppy Pose: For those who may not be up for a full inversion, this modified pose (arms and legs on a surface with hips raised) can also create beneficial space in the pelvis.
Typically, holding the inversion for one to three contractions can help prompt the baby’s movement.

Open Hip Positions and Upper Mid-Pelvis Openers:
Fire Hydrant Position: Lying with the belly down and hips open creates space for the baby to rotate.
Exaggerated Side-Lying: Using a peanut ball under the elevated leg while lying on the side encourages an optimal hip alignment.
These movements may be alternated between left and right, as many babies naturally rotate from the left side.
Upright Positions:
Transitioning into a seated “throne” position or an elevated lunge after open hip exercises helps guide the baby to drop into the pelvis properly.
We highly suggest incorporating a “Miles Circuit” that combines these movements for a comprehensive approach to support the baby’s rotation.

Working With Your Healthcare Provider
An important part of navigating labor is having an open conversation with your care team about your options. Ask questions like:
“What are your preferences and experiences with forceps versus vacuum-assisted deliveries?”
“How might each intervention affect my current labor and any future birth plans?”
“What are the specific signs that indicate we might need to change positions or consider an intervention?”
By discussing these topics, you can ensure that your birth plan is flexible and responsive to your unique labor progression while staying aligned with your personal comfort and long-term birth goals.
Preparing Prenatally for Optimal Labor
Exercise and Movement
Prenatal fitness isn’t just about staying active during pregnancy—it can also influence how smoothly labor progresses. Many of the exercises incorporated into our prenatal programs are designed to:
Strengthen the pelvic floor
Enhance hip mobility
Increase overall comfort during the final stages of labor
A great place to start is the MamasteFit Birth Prep Circuit!
Postpartum Recovery
If an instrument-assisted delivery is necessary, working with a pelvic floor physical therapist after birth is highly recommended. This can help address any additional stress or minor trauma to the pelvic floor or vaginal tissues, ensuring a smoother recovery post-delivery. To learn more about the pelvic floor and how to strengthen your pelvic floor for pregnancy, birth, and the postpartum, check out this video!
Final Thoughts
Labor is a dynamic and multifaceted process where the baby’s position plays a crucial role in shaping the experience of pushing and delivery. As highlighted in the Moments with MamasteFit podcast, understanding the nuances between occiput anterior and occiput posterior positions, recognizing the signs during labor, and knowing your intervention options can empower you to work with your healthcare team more confidently. Whether you’re exploring movement strategies like inversions and open hip positions or discussing instrument-assisted delivery options with your provider, the key is being informed and prepared.
For more insights into birth preparation, prenatal fitness, and recovery, explore our courses at MamasteFit and use code MOMENT10 for 10% off our offerings. Your journey through labor is personal, and having a well-rounded understanding of your options is a powerful tool in achieving a safe and satisfying birth experience.
Additional Resources
For more information on the pushing phase of labor, check out our recent podcast and Blog on pushing!
Prenatal Support Courses

Learn the science of pregnancy and birth to take the mystery of labor away! Understand why you are feeling what you feel, and learn strategies to confidently move through pregnancy and birth!
- 9h+ of Video
- Support Group
- Close Captioning

- 5 Workouts/Week
- Gym Workouts
- Self-Paced

Instructor
GINA
Workout on-demand with our prenatal fitness workout videos! Each workout is 30-40 minutes to follow along as you exercise at the same time!
- Birth Prep
- All Trimesters
- Mobility Work

Instructor
GINA
Find comfort and relief from pelvic girdle pain throughout your pregnancy and postpartum period! This program incorporates myofascial sling focused exercises to stabilize across the pelvic girdle joints.
- 3 Weeks
- On Demand Workout Videos to Follow






