Welcome to the latest episode of Moments with MamasteFit! In this mini episode, Roxanne and I explore the fascinating world of the placenta! We discuss its development, function, and how it ages throughout pregnancy. Learn about what the placenta does, how it acts as a filtration system for the baby, and the signs of its maturation. We also share insights on what influences placental health, discuss common prenatal tests, and offer tips on maintaining healthy placental function. Whether you’re expecting or simply curious, this episode provides a comprehensive look at one of pregnancy’s most essential organs.
What Is the Placenta and Why It Matters
The placenta is a temporary but critical organ that connects you and your baby. Through it, oxygen and nutrients flow from your bloodstream into your baby via the umbilical cord, while waste products are carried back into your body to be eliminated. It also acts as a barrier—filtering out many harmful substances and some pathogens to protect your little one.
Key functions of the placenta:
Nutrient and gas exchange via specialized units called cotyledons (you have 20–30 of these “filter pods”).
Waste removal to keep your baby’s environment safe and clean.
Immune protection by blocking certain bacteria and viruses.
Hormone production (e.g., hCG, progesterone) that supports pregnancy.

How the Placenta Develops: Weeks 4 to 12—and Beyond
Placental development happens in stages:
Weeks 4–8: Implantation begins around week 4; the placenta anchors to your uterine wall and starts building tiny blood vessels.
Week 8: Blood vessel networking accelerates as the placenta expands its reach.
Week 12: Villi formations (finger‑like projections that increase surface area) peak in number. From here on, both placenta and baby continue to grow in tandem.
Weeks 12–36: The placenta enlarges to match rising fetal demands—by term it will weigh around 1 lb (450 g).
By 36 weeks, the placenta reaches its maximum size and functional capacity. This leaves a built‑in “reserve” so baby’s growing needs remain met, even as maternal supply plateaus.
Placental Maturation and Signs of “Aging”
After 36 weeks, you may notice subtle signs of placental maturation—sometimes described as “aging.” These changes are often cosmetic and don’t necessarily signal dysfunction, but if they occur too early, they warrant attention.
Common placental aging features:
Calcifications (white, sand‑like spots) visible or palpable when you examine your placenta after birth.
Clumping of villi, leading to slightly reduced surface area.
Lower amniotic fluid volume (potentially causing oligohydramnios).
When to worry? If you see these signs on ultrasound before 36 weeks, or if amniotic fluid drops below safe levels, your provider may recommend closer monitoring or induction.
Monitoring Placental Function: Biophysical Profile & Non‑Stress Test
Rather than relying on due‑date milestones alone, modern obstetrics uses two key assessments to gauge placental and fetal well‑being:
An ultrasound evaluating:
Amniotic fluid volume
Gross and fine fetal movements
Fetal tone (practice breathing and stretching)
Each component is scored 0 or 2, for a total up to 8 (higher scores = healthier baby).
8/8: Excellent. 6/8: Continue monitoring; discuss fluid levels. ≤4/8: Consider induction.
Monitors fetal heart rate and contractions for 20–40 minutes.
Reactive (2 accelerations) = 2 points; non‑reactive = 0.
Combined with BPP for a full picture of placental reserve and fetal health.
Always remember: these tests inform a conversation, not a mandate. Your preferences, overall health, and risk factors shape any decision to induce labor.
Risk Factors That Can Stress Your Placenta
Certain conditions can chronically strain placental function, potentially impairing growth or hastening maturation:
Smoking: Reduces blood flow, increasing risk of small‑for‑gestational‑age babies.
Preeclampsia or chronic hypertension: High blood pressure damages placental vessels.
Diabetes (preexisting or gestational): Poorly controlled blood sugar alters placental metabolism.
Nutrient deficiencies: Low iron (anemia), vitamin D, calcium or zinc may impede placental efficiency.
Infections: Group B strep and other bacterial/viral infections can trigger inflammation and preterm birth.
If you have any of these concerns, work closely with your provider to monitor placenta and fetal well‑being.
Strategies to Support Healthy Placental Development
While some factors are beyond your control, there are proactive steps you can take to nurture your placenta:
Routine prenatal care: Early and regular check‑ups catch complications before they escalate.
Moderate exercise: Aerobic activity (e.g., daily walks, prenatal fitness classes) during the first 20 weeks boosts placental volume and vascular growth.
Balanced nutrition: Focus on folate, B12, zinc, iron‑rich foods, and plenty of fruits and vegetables—plus the occasional treat for mental well‑being!
Blood sugar management: For gestational diabetes, work with a dietician to maintain stable glucose.
Avoid tobacco and limit alcohol: Even one glass of wine before the placenta fully embeds (around week 4) probably won’t harm, but best practice is to abstain.
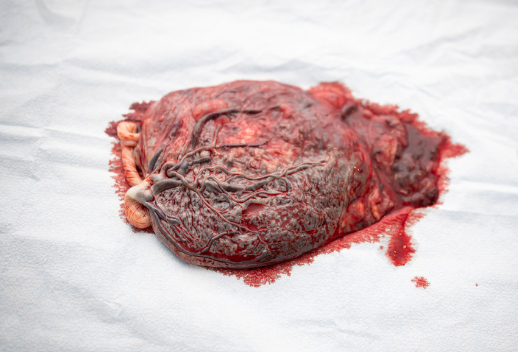
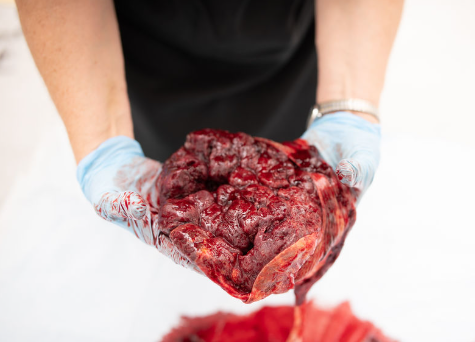
A Post‑Birth Tour: Getting to Know Your Placenta
After delivery, peel back the curtain on your body’s superstar organ:
Fetal side (Shiny Schultz): Smooth, glassy surface with a tree‑like network of vessels. Some mothers keep this side for placental art or photography!
Maternal side (Dirty Duncan): Rich, meaty texture where the placenta was attached to your uterine wall.
Cotyledons: Count the 20–30 little lobes on the Dirty Duncan side; missing pieces can lead to postpartum bleeding if any are retained.
Beyond inspection:
Placenta planting: Many parents bury the placenta with a tree as a living memorial.
Encapsulation or smoothies: Popular ways to consume for potential hormonal and nutritional benefits—though it remains your choice.

Final Thoughts
Your placenta is far more than a temporary attachment—it’s a dynamic, life‑sustaining organ that adapts alongside your baby. By understanding its development, recognizing signs of maturation, and leveraging tests like the BPP and NST, you can partner with your provider to make empowered choices about induction and ongoing care.
For more insights into birth preparation, prenatal fitness, and recovery, explore our courses at MamasteFit and use code MOMENT10 for 10% off our offerings.
Additional Resources

Biophysical Profile Test: Must-Know Insights for Your Baby’s Health
If your healthcare provider has recommended something called a “biophysical profile” during your pregnancy, you might be left wondering what it is and why it’s

Nonstress Test: Must-Know Insights for Your Baby’s Health
If you’re pregnant and have been told you need a non-stress test (NST), you might be wondering what that actually means, what doctors are looking

Exercising Throughout Pregnancy: Placental Benefits
Did you know that exercising in the first half of your pregnancy can positively impact your baby’s placenta function? But, how can you feel confident
Prenatal Support Courses

Learn the science of pregnancy and birth to take the mystery of labor away! Understand why you are feeling what you feel, and learn strategies to confidently move through pregnancy and birth!
- 9h+ of Video
- Support Group
- Close Captioning

- 5 Workouts/Week
- Gym Workouts
- Self-Paced

Instructor
GINA
Workout on-demand with our prenatal fitness workout videos! Each workout is 30-40 minutes to follow along as you exercise at the same time!
- Birth Prep
- All Trimesters
- Mobility Work

Instructor
GINA
Find comfort and relief from pelvic girdle pain throughout your pregnancy and postpartum period! This program incorporates myofascial sling focused exercises to stabilize across the pelvic girdle joints.
- 3 Weeks
- On Demand Workout Videos to Follow